Development of internal reproductive organs
- This section contains information on:
> Formation of the sexual ducts
The embryo lays down the rudiments of two complete sets of internal reproductive structures, one male and one female. In each sex, hormones stimulate one set to grow, while the other set is suppressed and degenerates.
The gonads — testes or ovaries — need to be connected to the rest of the body so that hormones and gametes (sperm or oocytes) can be transported away. This involves a system of tubes (ducts) and storage vessels (glands or vesicles).
These internal reproductive organs — that is, the sex-specific reproductive glands, ducts and organs other than the gonads — develop in a different way to the gonads and external genitals.
Two complete sets of tubes, male-type and female-type, are initially laid down; the growth of one of these is promoted, while the other is encouraged to disintegrate, depending on which chemical signals and hormones are produced by the developing gonads.
The embryonic structures that give rise to the internal sex organs in males are called Wolffian ducts (blue in the diagram below). The structures in females are called Müllerian ducts (pink in the diagram below). Both sets of ducts are attached at one end to the developing gonads, which are positioned next to the kidneys, and converge at the other end near the base of the genital tubercle, making a V-shape.
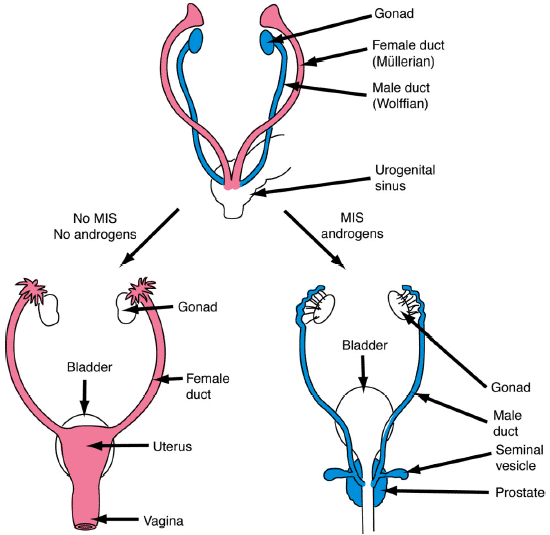
(Image from http://web.uvic.ca/~lalonde/psyc335/notes/lecture03.html)
The right-hand diagram illustrates how in males, the Müllerian ducts regress under the influence of a chemical signal called anti-Müllerian hormone (AMH) or Müllerian inhibiting substance (MIS), produced by the Sertoli cells of the developing testes. By about the 12th week of gestation, androgens (testosterone) produced by the testes promotes the development of the Wolffian ducts into spermatic ducts that connect the testes to the urethra so that sperm can be ejaculated. Later, the seminal vesicle and the prostate gland also form along these ducts to store sperm and seminal fluid.
The left-hand diagram illustrates how females, it is the Wolffian ducts that wither and disappear, while growth of the Müllerian ducts is promoted, ultimately resulting in the formation of the oviducts, Fallopian tubes, uterus, cervix, and upper vagina.
Because testes are initially formed inside the abdomen of the embryo, they need to migrate downwards into the scrotum, usually before birth — a process known as testicular descent.
Testicular descent is thought to occur in two phases.
In the first phase (11-15 weeks), the testes migrate down the abdomen under the influence of hormones Insulin-like factor 3 (INSL3) and, possibly, anti-Müllerian hormone (AMH or MIS), produced by the Leydig cells and Sertoli cells of the testes, respectively.
The second phase, starting at 25 weeks, involves the testes exiting the abdominal cavity via the inguinal canal, a ring at the groin through which they enter the scrotum. This phase depends largely on a number of chemical signals including testosterone, produced by Leydig cells of the testes.
Testicular descent is usually complete by the time of birth, but in some boys may not be completed until several months later.
A final note is that each testis must descend independently of the other, and so it is possible that one testis may find its way into the scrotum while the other remains undescended.
Further reading:
Hughes, IA and Acerini, CL. Factors controlling testis descent. European Journal of Endocrinology, volume 159 Supplement 1, pages S75-82, 2008 (open access).
-----------------------------------------------
Last updated: 5 August 2021 PK
Edit history: Author P. Koopman 9/2012; revised PK 5/2013, 10/2013, 7/2015