Hypospadias
What is hypospadias?
Hypospadias (pronounced high-poh-spay-dee-us) is a condition resulting from atypical development of the penis. Instead of the urinary tube (urethra) opening at the tip of the penis, it opens anywhere along a line on the underside.
In 50-75% of hypospadias cases, the urethra opens somewhere on the head of the penis, but not the very tip; this condition is categorised as first-degree or primary hypospadias. Second-degree or secondary (when the urethra opens on the shaft), and third-degree or tertiary hypospadias (when the urethra opens on the perineum, at or behind the level of the scrotum) occur in up to 20 and 30% of cases respectively.
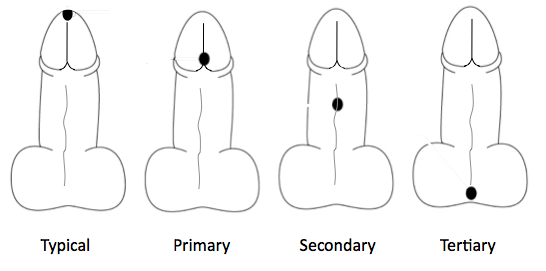 Hypospadias is often associated with downward curvature of the penis, a condition known medically as chordee.
Hypospadias is often associated with downward curvature of the penis, a condition known medically as chordee.
What causes this?
As the penis develops during embryonic life, the urethra forms by "zipping up" a flat piece of tissue to form a tube, starting at the base of the penis and finishing at the tip. A disturbance of the molecular signals that direct this process can lead to incomplete tube formation that finishes before it reaches the tip of the penis. These signals can come from hormones or from the direct action of genes involved in the “zipping” process, and a number of gene defects have been identified as causing hypospadias. Also, the increasing frequency of hypospadias in the population in the last 60 years suggests the involvement of additional, environmental factors (such as chemicals, additives or food-derived hormones used in large quantities since World War II).
How common is it?
Hypospadias is one of the most common birth defects in boys – estimates suggest that between 1 in 100 and 1 in 250 boys are born with hypospadias.
In recent decades, the frequency has risen to 2-4% of male births in some regions of some countries. This increase in such a short time span, together with the geographical variation in frequency, suggests that factors in addition to simple genetics must be involved, because purely genetic diseases do not change in frequency so quickly.
Is it a cause for concern?
Hypospadias can lead to self-consciousness associated with the appearance of the penis, and in some cases makes it difficult for boys to urinate standing up. Depending on the degree of the hypospadias, it may interfere with a male’s fertility if semen cannot be delivered into the vagina during heterosexual intercourse.
Hypospadias may be isolated (that is, occur in the absence of other irregularities of sex development), or may be part of a more complex syndrome of sex characteristics.
Perineal (tertiary) hypospadias, and in some cases lesser degrees of hypospadias, may be a symptom of variations in other aspects of sexual development and require investigation.
What is usually done about it?
Milder forms of hypospadias are usually corrected by surgery before the age of 18 months, under a general anaesthetic. It involves using a piece of foreskin to make a tube that can extend the urethra to reach the tip of the penis. The surgery usually also corrects chordee, if present. Usually only a single operation is necessary. Correction of hypospadias has become one of the most common types of pediatric surgical operation. Almost all parents elect to have the hypospadias corrected because the surgery is relatively simple and allows the boy to avoid any physical or psychological complications associated with having an unusual penis. There are normally no additional requirements such as ongoing counselling, medication, etc.
Readers are advised to seek the services of a qualified medical practitioner when considering any diagnostic or treatment options. See Disclaimer.
Further reading
Useful information and diagrams relating to hypospadias can be found at
https://www.rch.org.au/kidsinfo/fact_sheets/Hypospadias/
https://www.cdc.gov/ncbddd/birthdefects/hypospadias.html
-----------------------------------------------
Last updated: 6 August 2021 PK
Edit history: Author P. Koopman 9/2009; revised PK 9/2012, 5/2013, 10/2013, 7/2015